Table of Contents
Have you ever experienced a headache or eye pain along with a toothache? And you wonder if there is any relation that exists between them.
This article will not only explain why toothache causing headaches and eye pain but also give insight into the key areas where you may experience migrating pain in case of dental problems. Moreover, we also offer some home remedies to prevent toothache and discuss when you should visit your doctor.
Tooth pain leading to headache and eye pain: What is the connection?
In many cases, headaches or eye pain that we sometimes experience stems from dental problems. So what is the link between them? Let’s explore it in more detail.
Can tooth pain lead to headaches?
Yes. Due to many reasons, toothache can lead to headaches and even more severe migraines (1). The reason behind this is the complex anatomy of our nervous system that supplies more than one body part with the same nerve.
Cranial nerves, which are the nerves that supply the head and face, are arranged in a way that pain in one part may be referred to as pain in other parts. One such example is when dental pain caused by the trigeminal nerve, which also supplies sensory to the head and face, thus, it leads to pain in these areas too (2).
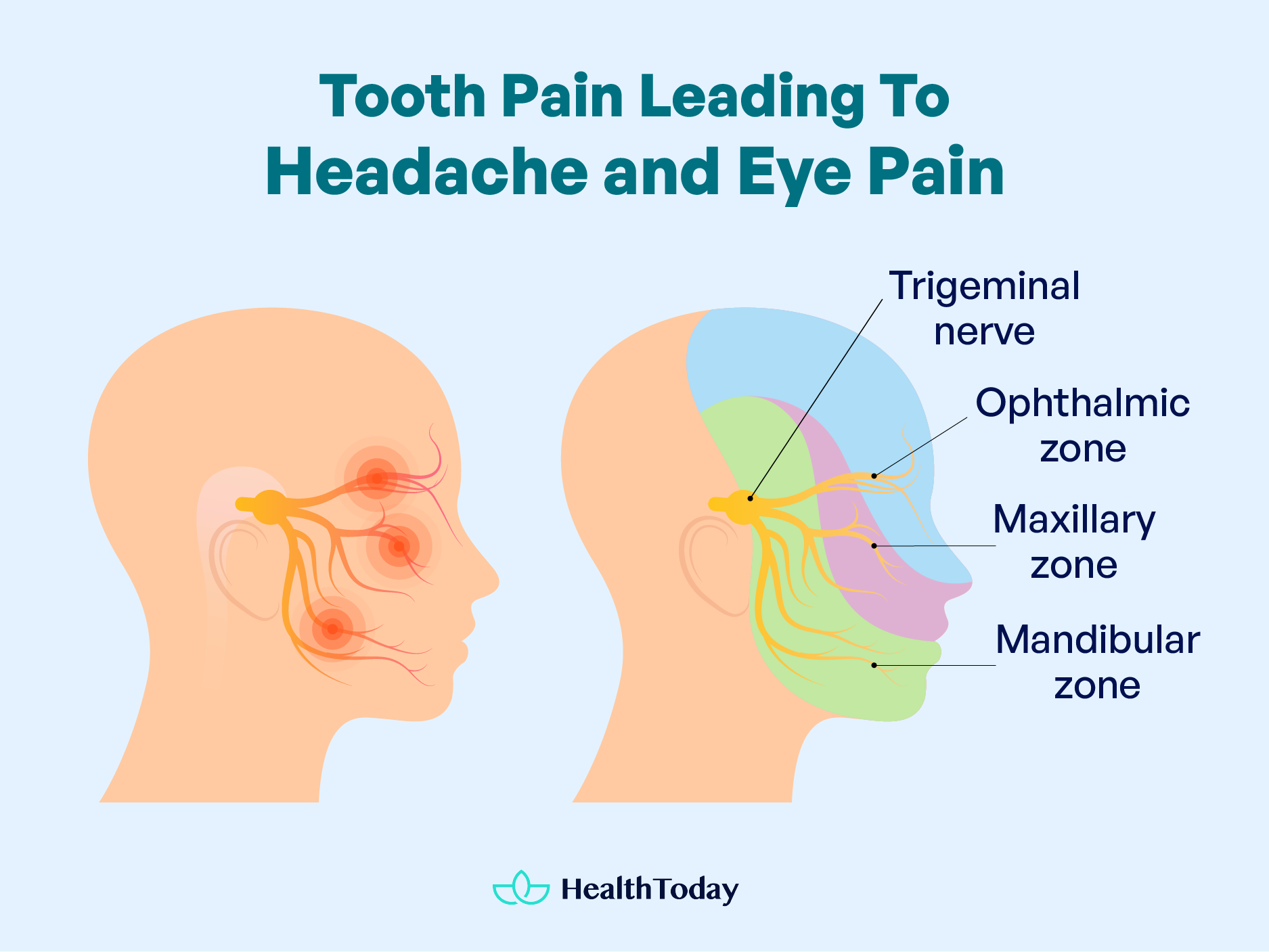
Individuals with dental problems may sometimes report headaches or even migraines, which are throbbing one-sided headaches with or without auras, for years (3).
The core reason for this association is the trigeminal nerve, the most vital cranial nerve that supplies a major portion of the face, head, and oral cavity. It is the same nerve that is also involved in migraines. Infection in the territory of the trigeminal nerve can lead to headaches (3).
Here are some easily diagnosed dental problems that can cause headaches and can be identified with simple examinations (3):
- Cavities, holes, or tiny openings: They are formed in the damaged areas of your teeth and result from sugary foods, oral germs (bacteria), improper cleaning, etc. They are also known as caries or tooth decay (4).
- Bone loss due to periodontal disease: Periodontitis is the inflammation of structures surrounding the teeth, such as gums. It can form plaque, tartar, and bacterial infection, which, if it goes deeper into the tooth, can result in bone loss (5).
- Dental abscess: An abscess is a pocket of pus formed inside a tooth or in the structures surrounding the teeth. The abscess at the end of a tooth is also known as a periapical abscess or periodontal abscess in the gums (6).
- Tooth cyst: Cysts are cavities with a covering formed from the same cells as the one involved in teeth formation. Their formation is due to inflammation or developmental problems inside a mother’s womb (7).
- Pulp infection: Pulp is the soft inner tissue of your teeth. Pulp supplies nutrition to the outer layers of teeth. Pulp infection is known as pulpitis— inflammation of the pulp (8).
- Tumors: Dental tumors, or odontogenic tumors, are abnormal tissue formed inside the teeth or structures surrounding them. They are often benign and have slow growth (9).
- Temporomandibular joint disorder (TMD): This is a condition that has various reasons, from genetics to psychological issues. It is due to the strain in muscles surrounding teeth and joint dysfunction in chewing. TMD is a major contributor to headaches. It often goes away on its own. It responds well to conservative measures, such as stress-relaxing techniques, jaw exercises, and over-the-counter painkillers (10).
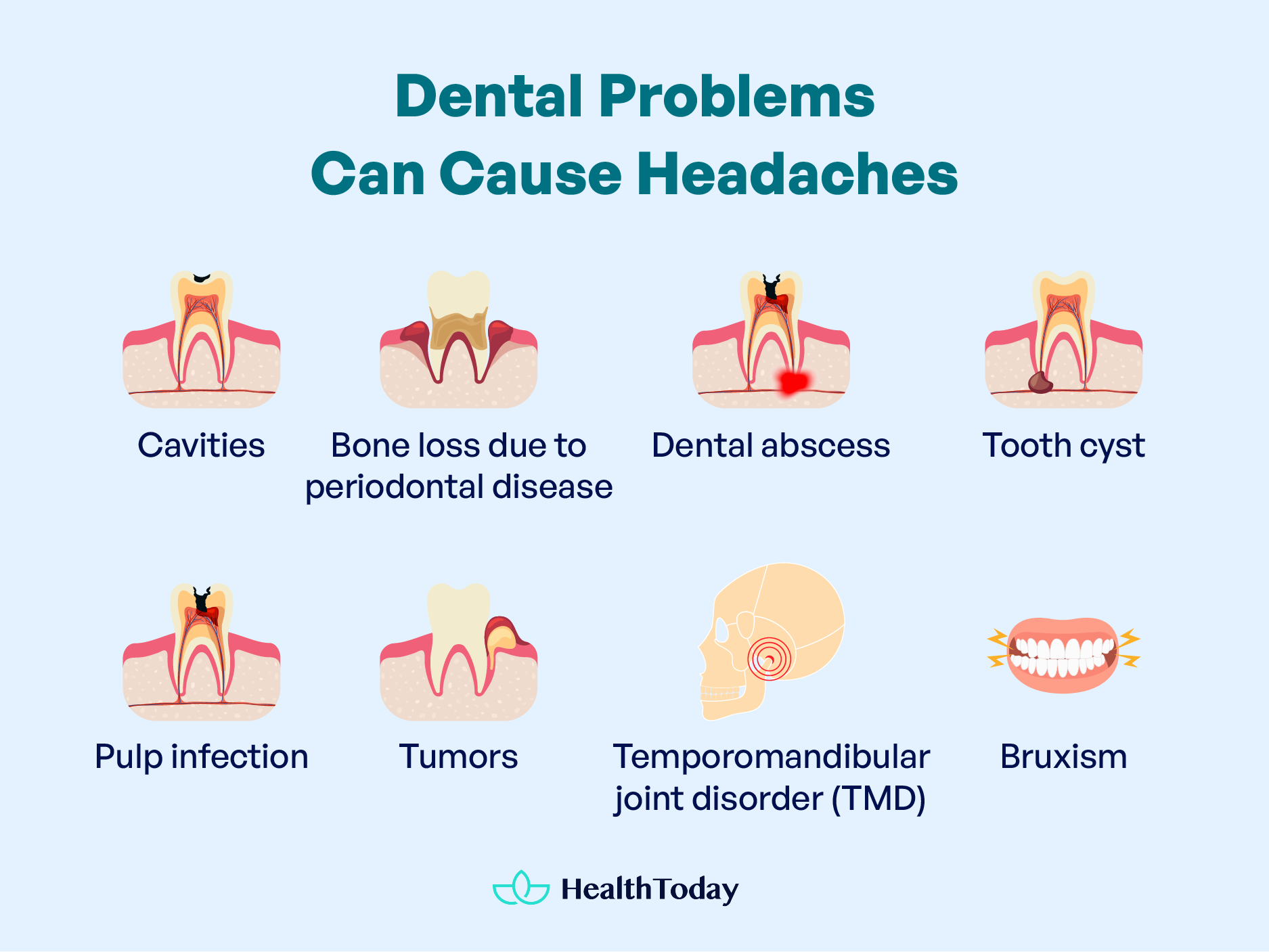
Another common dental problem that can cause headaches and often remains undiagnosed is bruxism. Bruxism is also known as tooth grinding. Sometimes you may grind your teeth during sleep and are unaware of it, called sleep bruxism. In other cases, you may be aware of grinding your teeth, called awake bruxism. Stress is the main cause of bruxism, apart from other minor and rare etiologies (11).
Tooth pain and eye pain
Toothache can be felt in the eye, known as “referred orbital eye pain.” Various medical etiologies in teeth, jaw, and facial joints can cause eye pain, watery eyes, strain, blurry vision, and sensitivity to light. Eye pain due to dental or bite problems can be felt as pain around or behind the eyes (12).
The reason for this association is the same as the link between headache and toothache, the trigeminal nerve. The trigeminal nerve provides sensory nerve branches to the upper jaw and the area around the eye, and sensory and motor nerve branches to the lower jaw. Thus, when one branch is impacted, it can refer pain to the other branches as well (12).
Sometimes not only is pain transmitted to the eyes, but infection can travel from the mouth to the eyes through the floor of orbits. If this remains untreated, it can lead to serious complications, as listed below (13).
Toothache can cause the following eye diseases if pain or infection is transmitted from the oral cavity (14):
- Ophthalmia: this term is used for eye inflammation, especially conjunctivitis
- Defective vision
- Contraction of visual field
- Orbital cellulitis: Infection and inflammation of the whole orbit; a structure that contains all eye structures
One potential complication of tooth infections leading to eye injury is Glaucoma, which has been well-studied (16, 24). Only a very small portion of all Glaucoma cases result from complications from tooth infections. Glaucoma is the second leading cause of blindness in the world. It slowly affects the vision and is also known as the “silent thief of vision.” It destroys the optic nerve that is linked to vision (15).
A large study examining the risk of various periodontal diseases and acute open-angle glaucoma (OAG) found that tooth loss in the last two years was associated with an increased risk of primary open-angle glaucoma (POAG). However, more studies are needed to determine this connection (16). The possible mechanism is tooth infections can activate our immune defense system, which may release chemicals that cause glaucoma. Another proposed mechanism is inflammation which causes dysfunction in the lining of blood vessels due to tooth problems (16).
The route that dental infections take toward the eye is usually through the maxillary sinus, which is a hollow space behind your cheeks (13).
Even tooth infections can lead to sinusitis—an infection of the sinus that can ultimately travel towards the eye (13, 22). Sinusitis, with or without dental infections, can lead to orbital cellulitis (infection and inflammation of eye orbits) (23). Sinusitis can also cause headaches, known as sinus headaches, which is another way toothache can cause headaches (17).
Toothache can lead to headaches via the trigeminal nerve, which carries a pain sensation from both areas. It can also cause eye pain for the same reason; not only pain but infections can travel from teeth to eyes. Dental problems such as cavities, abscesses, periodontitis, tooth cysts, and bruxism can cause headaches. Sometimes migraines are due to occult dental problems. The spread of infection to the eyes can distort vision and orbital cellulitis (eye infection).
“I have a toothache and a headache”: When should you see your doctor?
Headache due to toothache, as already discussed, is a common manifestation, but the question is when should you visit your doctor for this problem? Toothache that lasts for two or more days, or is associated with other systemic symptoms should be a sign for you to visit your doctor (1).
Severe toothache, fever, headache, or chills, demands urgent attention as it may indicate the spread of dental infection to other body parts (1).
If pus drains from your teeth and other symptoms as described above, it is a sign of dental abscess, and you need urgent treatment (18).
If there is swelling on the face or difficulty in swallowing or breathing, it’s a sign of the deeper spread of dental infection, and you should see the doctor promptly (18).
Maxillary sinusitis may also cause toothache. If toothache and headaches are due to sinusitis, a doctor may prescribe medication to help cure it, especially if it has lasted multiple days. Facial pain over cheeks is a strong sign of maxillary sinusitis apart from toothache and headache (2).
Eye swelling, along with toothache, facial pain, fever, and headache, may point towards orbital cellulitis, which can become a serious complication if it develops. Orbital cellulitis is an infection inside the eye. If the dental infection is not treated promptly, it can spread to the brain or develop an abscess (13).
Defective vision, blurriness, eyelid swelling, watery eyes, and ophthalmia (inflammation of the conjunctiva) in case of dental infections require you to visit your doctor. These symptoms indicate the infection has spread from the oral cavity to the eyes (14).
Poor jaw alignment or biting patterns (When your upper and lower teeth do not match properly) also lead to long-term headaches. It puts strain on jaw muscles and joints, resulting in chronic pain. This pain may linger on for a long time and then subside for some time just to reappear. It’s better to resolve it by getting your bite aligned through a dentist early in life otherwise, it will keep teasing you for a lifetime (12).
Coping with tooth, head, and eye pain: Preventions
You may wonder if we can prevent the spread of dental infections to other facial areas. And what we can do to relieve headaches or eye pain associated with toothache at home? Here are home remedies and medical treatments for these cases:
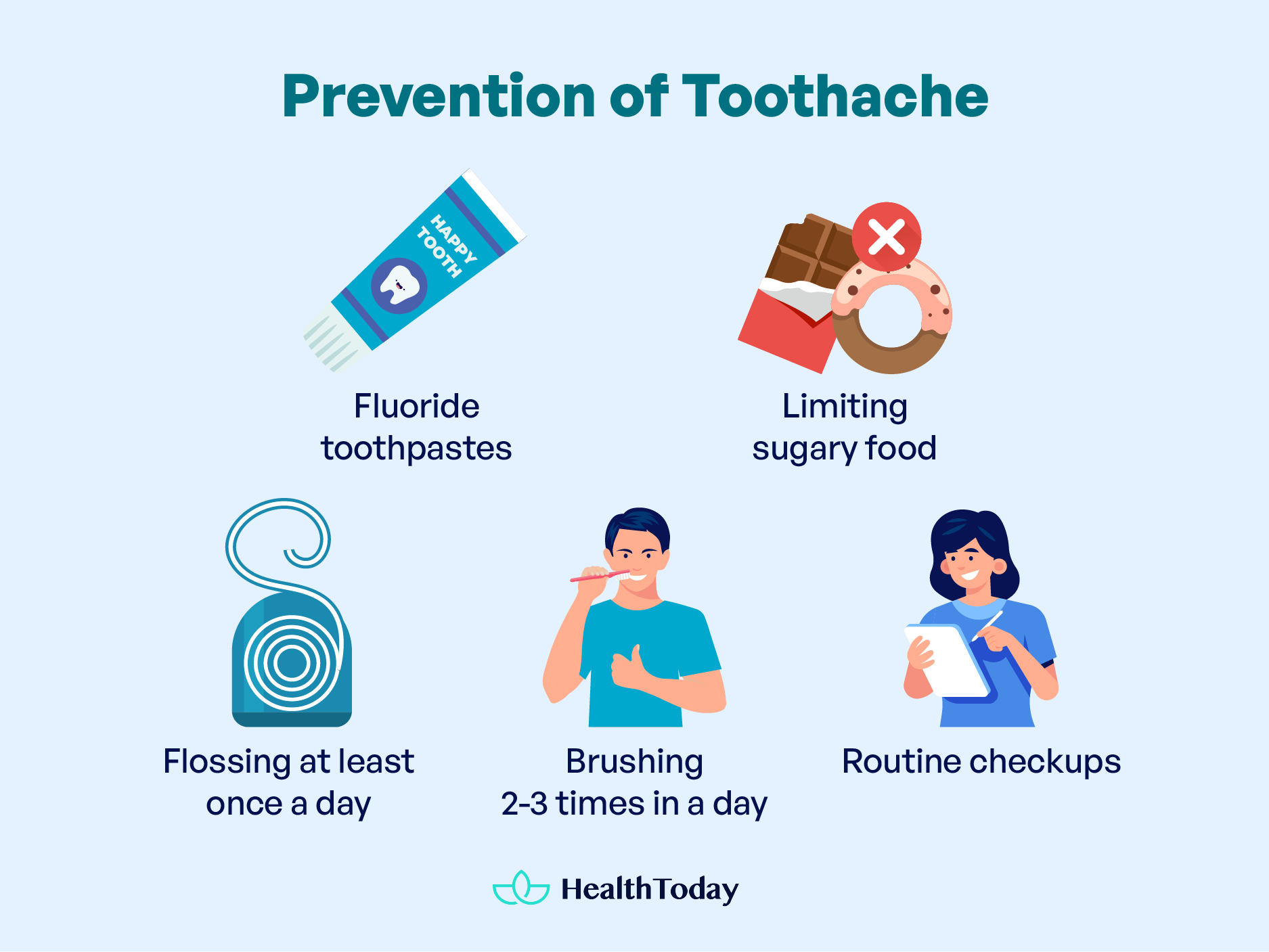
Prevention of toothache
It is impossible to prevent toothache completely because multiple micro-organisms reside in our mouths and can cause dental infections. Here are some things that can help you in lowering the risk of having a toothache (1):
- Use of fluoride toothpastes
- Limiting sugary foods
- Flossing at least once a day
- Brushing 2-3 times in a day
- Regular visits to dentists for routine checkups
Managing your conditions:
To manage your condition, it is important to recognize the signs early. These are simple tests that your healthcare provider may perform to identify the cause of dental pain (2):
- Palpation: Careful touching the area may help identify the problem.
- Mobility test: Prominent movement of the tooth held by a hand can indicate bone loss or issues in the tooth’s root. Please note that a small amount of mobility is present in normal teeth (<0.5mm).
- Probing: Probing the area around the gum may result in bleeding or visible pus if there is an infection or abscess.
- Pulp sensitivity test: If stimulating the pulp of a tooth with a dry ice stick results in a painful response, it indicates normal tissue. In contrast, if there is no response, it’s a sign of damaged pulp. Pulp is the portion of a tooth that supplies it with nutrition and nerves.
- Radiographic investigations: After a thorough examination, radiographs can help visualize the cause of dental pain clearly in most cases.
If a toothache develops, managing it as early as possible is the key to controlling its spread to the eyes, sinuses, or other orofacial areas. Following are some medical treatment options for different causes of toothaches (1):
- Medications: painkillers and antibiotics can help combat dental infection at its earlier stages and control its spread and associated pain.
- Filling: In cavities, dentists usually fill the space to reduce the chances of bacteria growing there and damaging more parts of the tooth.
- Root canal: if the pulp of a tooth which provides nutrition to the teeth, gets infected or invaded by germs, it can cause severe pain as it has a lot of pain-carrying nerves. The root canal helps to remove the infected nerves and damaged areas.
- Crowns: for a fractured tooth or if there is a cavity so enlarged that it cannot be treated with filling, dental crowns may help.
- Dental extraction: it’s a last resort, but if the condition is not amenable to treatment, the dentist may have to remove the teeth, especially in cases of dental abscess or necrotic tooth that has a high chance of spreading beyond the oral cavity (3).
Bruxism or teeth grinding is another common condition that is not seriously harmful but can result in the wearing of teeth and long-term mild facial pain, as well as headaches. In this case, your healthcare provider may offer you stress reduction techniques in addition to a night guard to protect your teeth (11).
Home remedies
If your symptoms do not require urgent medical attention or if you are on the waiting list to get an appointment, some simple home remedies to prevent and treat toothache associated with headaches and orofacial pain include (1):
- Ice packs: wrap ice in a clean cloth and apply it outside of the affected area for some minutes. Ice helps to relieve pain, and it also constricts blood vessels, temporarily reducing inflammation.
- Salt water rinse: salt water works as a disinfectant and helps in combating toothache.
- Hydrogen peroxide: rinse with hydrogen peroxide after diluting it in water. It works in healing by fighting with oral germs. Please note, don’t use it without dilution.
Over-the-counter analgesics: Over-the-counter painkillers such as paracetamol or NSAIDS (e.g., ibuprofen) can relieve pain and even reduce inflammation in mild cases (19).
To prevent toothache, which is associated with headaches and eye pain, proper cleaning, regular flossing, and use of fluoride toothpaste are essential. When you visit a dentist, they may identify your problem with palpation, mobility tests, sensitivity tests, and radiographic investigations.
Different treatment options for toothache include painkillers, filling, root canals, crowns, and dental extraction. Home tricks that help with dental pain involve ice packs, salt water rinse, and over-the-counter analgesics.
What are the symptoms of a tooth infection spreading?
There are multiple symptoms of the spread of tooth infection, including facial pain (due to the spread to the sinus), headaches, ear pain, difficulty swallowing or breathing, swelling of the face, high-grade fever or chills. On rare occasions, there may be swelling of eyelids, blurry vision, protrusion of orbital contents (due to infection in orbits), (1, 2, 14, 18).
Why is my toothache spreading to my ear?
Sometimes damaged teeth can cause the surrounding area to get inflamed, and pain radiates to the ear. It is the proximity of the ear to teeth that makes a person feel as if he has an earache. Likewise, a primary ear infection can cause toothache for the same reasons (20).
Temporomandibular joint disorder (TMD) can cause toothache and earache simultaneously due to the involvement of surrounding muscles and joints (21).
Will brushing teeth help toothache?
Brushing helps to clean the teeth. It can help prevent toothache, but once toothache is developed, it needs to be treated, and brushing does not help in its treatment. However, you should continue brushing to stop the spread of dental infection (1).
Bottom Line
Problems related to the oral cavity can cause pains in the form of headaches or facial pain. This is because of the same nerves that supply these structures. You may experience migraines due to hidden dental problems. Dental infections, tumors, abscesses, cysts, TMD, and teeth grinding can all lead to orofacial pain, headaches, and eye pain.
Be aware of alarming signs and visit your healthcare provider in case of spread, which results in high-grade fever, chills, severe headaches, eyelid swelling, pus drainage from the teeth, facial swelling, etc. Medical treatments for toothache include medications, root canals, fillings, and dental crowns. Saltwater, hydrogen peroxide, OTC painkillers, and ice packs are effective home remedies for toothache. Try always to keep your mouth clean (oral hygiene) is the most important strategy in preventing toothache.
















Comments
0