Table of Contents
Can diabetes cause dizziness? ‘Dizziness’ is a common but sometimes vague symptom due to various causes and diagnoses. It sometimes makes diagnosing and treating dizziness challenging, even for experienced doctors.
This article delves into the connection between diabetes and dizziness and explains how lightheadedness may be an early sign of diabetes.
We also talk about how to stop dizziness from high blood sugar and provide tips for spotting and treating low blood sugar, a common symptom for people with diabetes.
Can high blood sugar cause dizziness and vertigo? Dizziness and diabetes explanation
Feeling dizzy is a common reason for medical visits—about 5% of walk-in clinics and 4% of emergency department patient visits complain about this, including two different underlying problems: “Dizziness” and “Vertigo.”
“Dizziness” differs from “vertigo,” a condition that feels similar but signals a set of very different diseases. The major features of vertigo (1) include:
- Having a persistent sensation that the environment is “spinning.” Patients complain the ceiling is moving even when sitting still.
- Having clear-cut attacks with a specific onset time
- Dizziness that feels worse when moving
While vertigo might result from problems affecting your brain or ears (2), dizziness may be due to heart problems or more general conditions such as an imbalance of ions in your body.
Based on the three signs mentioned above, you can help yourself or your doctor guess better if you have vertigo or dizziness.
Remember, not everyone’s condition can be correctly included in this simple and quick method, and many people have uncommon symptoms. You should visit a doctor if you are concerned about severe conditions.
Those who don’t have the above three signs of vertigo (people who have dizziness) might also experience hazy vision, confusion, or disorientation when standing up. In that case, diabetes might be a cause, especially for people older than 60, when 20% have severe dizziness that affects their daily lives (3).
Diabetic feeling sick and dizzy: What is happening?
Is dizziness a symptom of diabetes? Yes, and can be due to the following factors (3):
Hyperglycemia (high blood glucose)
Hyperglycemia occurs when your body can’t produce enough insulin (type 1 diabetes) or doesn’t use it properly (type 2 diabetes) (4), causing too much sugar to circulate in your blood.
Although glucose, a sugar in your blood, is a major fuel for your brain, too much of it is not necessarily good. High blood glucose can damage your nerves and cause inflammation and stress to your cells (5).
In a study on hyperglycemic symptoms in people with diabetes taking insulin, 26.9% experienced lightheadedness, and 22.4% reported dizziness (6), which often happens when they’re thirsty, have a dry mouth or simply do not feel right, which occurs about 80% of the time (6).
Hypoglycemia (low blood glucose)
Glucose is the brain’s fuel. When you have low blood sugar, it causes problems. When it takes a nosedive, it can quickly cause problems with your thinking and reflexes, like dizziness, seizures, fainting, or even permanent brain damage (7).
According to a study, about 11– 44% of those battling low blood sugar reported feeling dizzy (8). Other common symptoms of this condition include sweating, difficulty concentrating, and feeling weak.
Dehydration
In people with diabetes, when there is too much glucose in your blood, your kidneys may pee out more water from your body to get rid of the extra glucose (9).
Mild dehydration can trigger dizziness, which worsens in elderly people as they are less sensitive to thirst (10). Also, watch out for other dehydration signs like thirst, dry mouth, dark yellow and smelling urine, less pee, persistent fatigue, weakness, or muscle cramps (11).
Hypertension (high blood pressure)
For people with diabetes, they are twice as likely to have high blood pressure (12). High blood pressure can also cause dizziness in diabetes (3) and trigger heart attacks, stroke, bleeding, and other problems (13).
However, high blood pressure usually has no symptoms and is often found during medical check-ups. When it becomes severe, you may experience severe headaches, nausea, vomiting, confusion, vision changes, and nosebleeds (13), usually with systolic blood pressure greater than 180 mmHg or diastolic blood pressure greater than 120 mmHg (14).
Hypotension (low blood pressure)
As high glucose levels can damage your nerves, the autonomic nervous system, which helps regulate your blood pressure, can, thus, be weakened in diabetes. Therefore, it causes a drop in blood pressure and dizziness when standing up (“orthostatic dizziness”). This condition is known as orthostatic hypotension or postural hypotension (3).
Medications
To manage diabetes well, you must maintain stable blood sugar, blood pressure, and cholesterol levels (15). Medicines for diabetes may lower your blood sugar or pressure, but sometimes they can make it too low, causing dizziness (3, 16). Common causes are:
- Injecting the wrong type of insulin
- Injecting too much insulin
- Injecting directly into the muscle instead of under the skin (3, 17).
- Sulfonylurea medications for diabetes like Diamicron (gliclazide) and Amaryl® (glimepiride) (18).
- Diuretics and SGLT2 inhibitors for hypertension (19).
Hypoglycemia vs. Hyperglycemia-induced dizziness in diabetes
Blood sugar levels vary from one person to another. Yet, in general, if you check your levels at home, a typical target is 4‒7 mmol/L before eating and under 8.5‒9 mmol/L two hours after a meal (20).
Common symptoms when your blood sugar levels become lower than the normal range include (17, 21):
- Sweating
- Trembling
- Fatigue or muscle weakness
- Blurred vision (not that common, only about 20%) (8)
- Hunger
- Palpitations or pounding heart
- Slurred speech
- Numb lips
- Light-headed/dizziness
- Headaches
- Nervousness and anxiety
- Difficulty concentrating
- Drowsiness or sleepy
- Uncoordinated
- Cold sweats
- Slowed thinking
Hyperglycemia
Your blood sugar levels are high if your blood glucose is over 7 mmol/L (125 mg/dL) while fasting or over 11 mmol/L (180 mg/dL) two hours after eating (22, 23). For people diagnosed with diabetes, there are a few possibilities (4):
- Your diabetes does not respond well to your current medications
- You eat more or exercise less than you should
- You have mental or stress from an illness, like a cold or flu
- If the symptoms commonly happen around 4-5 am, you may experience the dawn phenomenon, where your body has a hormone surge around that time, including cortisol and growth hormones (24)
Symptoms of high blood sugar usually develop gradually and become apparent when the level is very high (22), called Hyperosmolar Hyperglycemic Syndrome, or HHS (25). You might feel thirsty, have a dry mouth and sticky lips, pee frequently, and have unintentional weight loss (6, 21). That’s why high blood sugar and dizziness often go hand in hand.
Hypoglycemia
For those with diabetes, hypoglycemia means a blood sugar level lower than 70 mg/dL or 4 mmol/L (16, 17). For non-diabetics, your threshold is around 55 mg/dL (26).
Low blood sugar typically affects people with diabetes taking insulin or other diabetes medications. It is not likely to happen in people without diabetes (16), but if you experience symptoms of low blood sugar for no reason, you should plan for a checkup: there might be other rarer reasons (27).
For people with diabetes who experience symptoms of low blood sugar, it is often called an insulin reaction or insulin shock (17, 28). Besides feeling dizzy, other possible symptoms include (16, 17):
- Shaking and trembling
- Nervousness or anxiety
- Sweating, chills, and clamminess
- Difficulty concentrating
- Confusion or irritability
- Fast heartbeat or palpitations
- Feeling hungry
- Nausea, skin turning pale
- Feeling sleepy
- Slurred speech
- Tingling or numbness around the lips and mouth
In rare occasions, seizures or coma may occur, so it is important to have someone nearby who knows your condition well.
On average, a person with type 1 diabetes may have up to two episodes of mild low blood sugar each week. If you count the ones without symptoms and those that happen at night – nocturnal hypoglycemia, the number might be higher (17). Hypoglycemia is also a problem for type 2 diabetes. In a study, 45% and 6% of those with this type experienced mild-to-moderate and severe hypoglycemia, respectively (28).
Can high blood sugar cause vertigo?
Vertigo is a feeling of the environment moving around you even when you remain still. It makes you feel disoriented, unsteady, lightheaded, and even pass out (3, 29).
Many people describe vertigo with words similar to dizziness, but it is a very different set of problems.
Vertigo can happen when your vestibular system is not working correctly because of infection, inflammation, drug use, or many other possibilities.
Vertigo and diabetes are closely linked. Long-term diabetes with high blood sugar can damage the nerve cells in your inner ear, causing peripheral vertigo. This is why people with diabetes often complain about dizziness; many may feel lightheaded when standing up. Therefore, diabetes can sometimes make you feel off balance.
According to a study, 84% of those with type 2 diabetes had an abnormal test result for at least one component of the inner ear vestibular system (2, 3). Another study shows those with diabetes were 70% more likely to have balance problems. In these cases, the chance of falling was 12 times higher (30).
Those with diabetes tend to experience benign paroxysmal positional vertigo (BPPV) than non-diabetic people (3). BPPV happens when tiny crystals in your inner ear move out of their normal position (only when you change position), leading to vertigo for typically less than a minute (2, 29, 31). Those with diabetes are prone to postural hypotension (32).
A study found that 22.9% and 16.2% of people with type 1 and type 2 diabetes, respectively, had this condition (3). A study also showed that those with diabetes and postural hypotension had a 2.2 times higher mortality rate than those without diabetes (32).
Diabetes and lightheadedness often go hand in hand, with various factors playing a role. Fluctuations in blood sugar and pressure, both high and low, can all lead to dizziness. Dehydration and potential side effects of medications also play a part. Plus, vertigo and diabetes can also closely link to diabetes.
Is dizziness after eating a sign of diabetes?
Aside from diabetes, multiple factors can make you feel dizzy. However, if you have diabetes or are at risk, experiencing dizziness after a meal could be an early sign.
Can eating make you dizzy?
Dizziness from eating can imply diabetes, but not always. However, you should be careful about this symptom: It may be a sign of low blood pressure or other underlying conditions.
Reactive hypoglycemia
Blood sugar usually rises after eating carbs. Thus, those feeling dizzy before a meal often feel relief afterward. However, if you have low blood sugar 2‒5 hours after eating, it can be reactive hypoglycemia (RH) causing dizziness (33).
When you have diabetes, your body doesn’t manage insulin efficiently after meals, leading to an initial spike in blood sugar followed by a delayed insulin response, potentially causing excessive insulin release later (33).
If your blood sugar plummets after consuming glucose for 4‒5 hours but you don’t have diabetes (your fasting blood glucose is too high, but not high enough to be called diabetes), you might have trouble responding to insulin. This condition is known as prediabetes (33, 34).
Your eating style matters
Eating habits may trigger low blood glucose levels, including (17, 20, 26):
- Missing a meal or not getting enough carbs.
- Being sick and unable to eat or keep food down.
- Exercising intensely.
- Overindulging in sugary or starchy food. Quick glucose spikes can set you up for hyperglycemia later. Liquid carbs are absorbed much faster than solids.
- How much fat, protein, and fiber included in your meal can affect the absorption of carbs.
- Drinking too much alcohol or with an empty stomach.
- Missing a dose of your diabetes medication or taking an incorrect dose.
Postprandial hypotension
In some scenarios, your blood pressure drops suddenly after eating, which is called postprandial hypotension (PPH). Technically, PPH is when systolic blood pressure drops by 20mmHg or more within two hours of eating (23, 35).
Experts are unsure what causes PPH, but one possibility is that your body’s response to blood pooling after a meal falls short (35).
PPH can cause dizziness, fainting, and falls. It is common in elderly adults and those with diabetes, hypertension, Alzheimer’s, and Parkinson’s (23).
Other causes of dizziness
Dizziness isn’t always a direct result of diabetes. Sometimes, it’s tied to various dizziness-inducing conditions, whether diabetes-related or not:
- Anxiety disorders, like panic attacks or agoraphobia (29).
- Anemia is when your body doesn’t have enough red blood cells to carry oxygen, causing balance issues (29).
- Neurological conditions like Parkinson’s disease, Ménière’s disease, multiple sclerosis, or peripheral neuropathy trigger disequilibrium (29, 31).
- Malnutrition, motion sickness, Addison’s disease, or a tumor in the pancreas may lead to episodes of hypoglycemia (16).
- Frequent infections, like thrush, bladder infections (cystitis), and skin infections, can trigger hyperglycemia (20).
- Maternally-inherited diabetes and deafness, a mitochondrial disorder (3).
Sometimes, dizziness is also a side effect of medication (3):
- Antibiotics like quinolones, fluoroquinolones (e.g., ciprofloxacin), macrolides (e.g., erythromycin), and aminoglycosides (e.g., gentamicin)
- Antifungals, such as amphotericin B and fluconazole
- Statins for lowering blood cholesterol levels
- Neuropathic pain relievers like amitriptyline, duloxetine, gabapentin, and pregabalin
Remember, dizziness isn’t something to wave away, especially as you age. Fortunately, in many cases, it can be prevented (31).
If dizziness keeps returning or sticks around, you should seek a doctor. It’s helpful to write down when it occurs before your appointment.
How to stop dizziness from high blood sugar?
If you feel dizzy occasionally and it goes away fast, there is nothing to worry about. But if dizziness becomes frequent, you should talk to your doctor (2), especially if you have diabetes.
Tackling the root cause will relieve dizziness. However, finding the right treatment, whether rehab, medications, or other options, will take time. You can also try home remedies to relieve discomfort temporarily (2).
Lifestyle changes
Hydration can be your most potent ally to stop dizziness. Sip on plain, calorie-free, and caffeine-free water. It will help quench your thirst and flush out excess glucose, wreaking havoc in your system (10, 20). A doctor can check if you need an electrolyte boost like potassium or salt (13, 31).
It’s best to consult your dietitian to change your meal plan and prevent sugar surges (4). You can also try the Mediterranean diet or intermittent fasting under medical supervision (36, 37).
Exercise can help decrease blood sugar levels. Consider fueling with carbs before, during, or after your workout or adjusting your insulin dosage (4, 38). Staying hydrated is vital for peak performance (10).
Moreover, if your blood glucose spikes above 240 mg/dL, check your urine for ketones. If they’re present, hold off on exercise, as it could increase your sugar levels (4).
If exercise and dietary changes are ineffective, consider changing the dosage or timing of your medication (4).
What to do if a diabetic feels dizzy?
The simple way to tackle dizziness is to try home remedies. Here are some natural remedies you can try.
Honey
Stone Age paintings show that honey has been a remedy for over 8,000 years. Ancients used it to treat health problems like fatigue, dizziness, and wounds. Plus, it has some protective effects for diabetes (39). Remember, as honey is also sugar-packed, you should use it with a small amount (40).
Ginkgo biloba
This Chinese herb can help with dizziness, especially equilibrium disorders, and vertigo, by improving blood flow to the brain. Only a few patients had mild side effects, like occasional headaches (41, 42). Steep some Ginkgo biloba leaves in hot water to harness its potential and savor the infusion.
Ginger root
Studies proved ginger’s effectiveness in preventing symptoms of dizziness and motion sickness (43). Ginger is also a promising adjuvant therapy for type 2 diabetes by improving insulin sensitivity (44). Toss ginger root into boiling water for 5 minutes to make a soothing ginger tea. A touch of honey is a tasty bonus.
Cinnamon
Cinnamon helps manage diabetes by reducing insulin resistance and improving liver enzymes in the long term. Besides, it could help with headaches, dizziness, stomach problems, and heart palpitations (45, 46).
Epley maneuver
The Epley maneuver is a set of simple head movements that can help alleviate symptoms of BPPV, or benign paroxysmal positional vertigo (2, 3, 47). However, keep in mind that this set of exercises is effective unless your vertigo is caused by BPPV. If you have BPPV, you should do these exercises three times daily until you don’t have positional vertigo in 24 hours (48).
BPPV can occur in the left or right ear, and the maneuver choice hinges on your affected ear (48, 49). Here’s a quick guide:
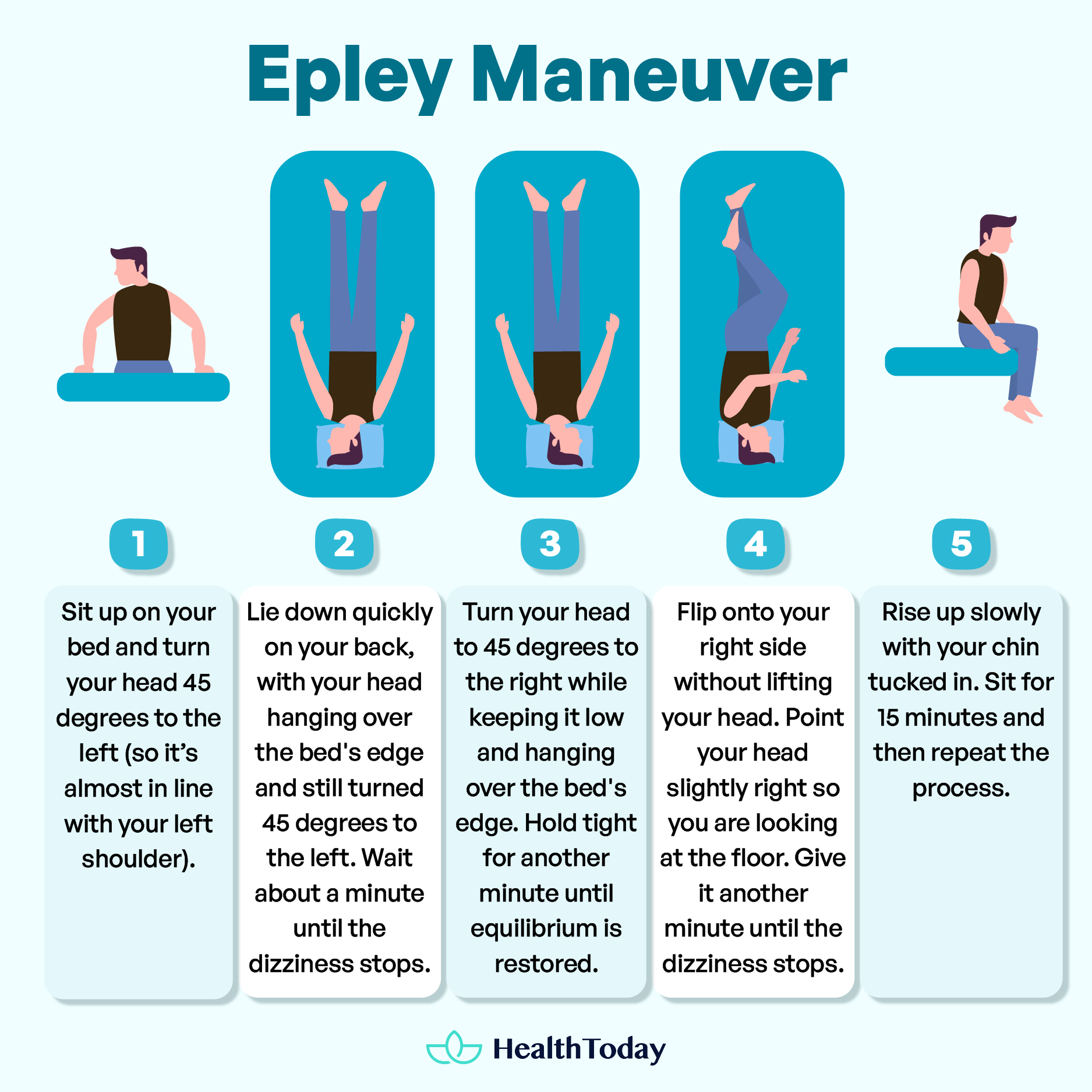
- Sit up on your bed and turn your head 45 degrees to the left (so it’s almost in line with your left shoulder).
- Lie down quickly on your back, with your head hanging over the bed’s edge and still turned 45 degrees to the left. Wait about a minute until the dizziness stops.
- Turn your head to 45 degrees to the right while keeping it low and hanging over the bed’s edge. Hold tight for another minute until equilibrium is restored.
- Flip onto your right side without lifting your head. Point your head slightly right so you are looking at the floor. Give it another minute until the dizziness stops.
- Rise slowly with your chin tucked in. Sit for 15 minutes and then repeat the process.
If you feel dizzy on the right side of your body or in your right ear, do the opposite of these directions (50).
Tackle a hypo
When dizziness strikes, it could be due to low or high blood sugar, and they share some symptoms. So, it’s better to check your blood sugar levels frequently, especially if you have signs of a hypo, such as being hungry, sleepy, shaky, sweaty, and dizzy (17).
A continuous glucose monitor (CGM) can alert you when your blood sugar levels plummet (17). Always keep some quick carbs—like glucose tablets, candies, or juice boxes—at hand (26, 38). Also, ensure your loved ones know how to handle severe drops in blood sugar levels (16).
To raise your blood sugar instantly, turn to the “15‒15 rule”. Eat 15 grams of carbs and check your blood sugar 15 minutes later. If it’s still below 70 mg/dL, repeat this until it reaches at least 70 mg/dL. Once your blood sugar improves, have a meal or snack to keep things steady (17).
To reach that 15 grams of carbs, here are some options (16, 17):
- 5 glucose or dextrose tablets
- 4 large jelly babies
- 4 ounces (1/2 cup) of juice or regular soda (not diet soda)
- 2 tubes of glucose gel.
- 1 tablespoon of sugar, honey, or corn syrup
- Hard candies, jellybeans, or gumdrops—check the label to decide the quantity.
Eating until you feel better sounds tempting, but it will help raise your blood sugar levels. Stick to small, measured steps (17). Once your symptoms improve, opt for foods that provide steady blood sugar levels, such as biscuits, sandwiches, or your next meal (16).
However, you should avoid foods with complex carbs or fats, such as chocolate, as they slow down sugar absorption, which you don’t want in this scenario (17).
Babies and children need less amounts of carbs, from 6‒10 grams. It’s best to discuss with your doctor to customize the approach (17).
Remember, in diabetes, sugary treats are usually avoided and only consumed in emergency hypo situations.
When to seek urgent medical attention?
Very high blood sugar levels can cause life-threatening complications, such as (20):
- Diabetic ketoacidosis (DKA): This is a big concern for those with type 1 diabetes, which can cause a diabetic coma. It happens when your body needs to break down fat for energy, releasing ketones. It usually happens with younger patients who forget to eat their meals after injecting insulin.
- Hyperosmolar hyperglycaemic state (HHS): This causes severe dehydration since the body tries to flush excess sugar. It usually occurs in older people with type 2 diabetes after an infection of the urinary tract or the skin.
If you have diabetes and experience any of the following symptoms along with dizziness, call your care team or dial 911 (or your local emergency number) right away (4, 13, 17, 22):
- Sickness or stomach pain
- Having a very dry mouth
- Rapid breathing or fast heartbeat
- Fruity-smelling breath (like pear drops)
- Confusion, irritability, or unable to concentrate
- Drowsiness or difficulty staying awake
- Feeling nauseous and vomiting
If a person with diabetes becomes unconscious because of dizziness, especially after drinking alcohol, put them into the recovery position after calling local emergency services (17, 51):
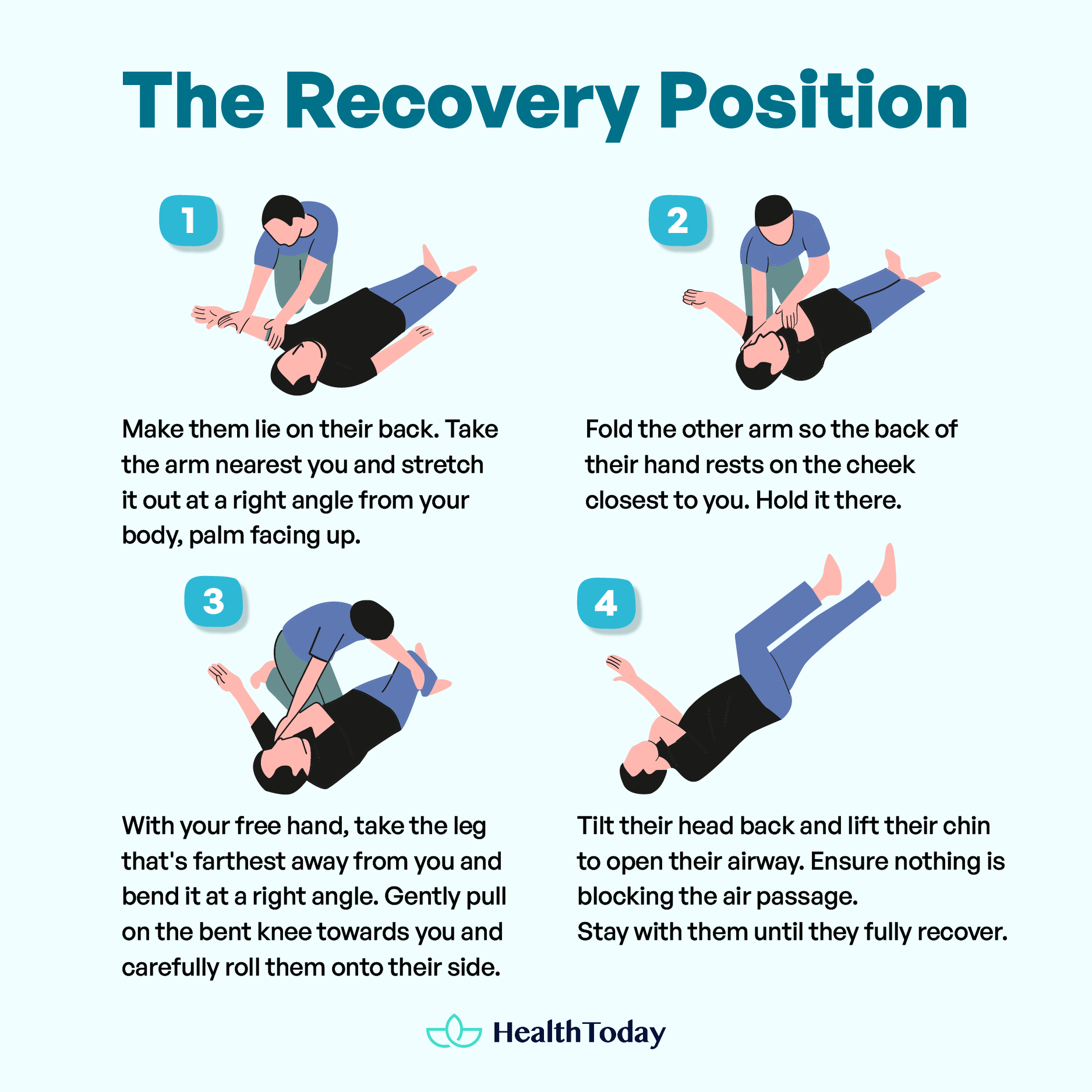
- Make them lie on their back. Take the arm nearest you and stretch it out at a right angle from your body, palm facing up.
- Fold the other arm so the back of their hand rests on the cheek closest to you. Hold it there.
- With your free hand, take the leg that’s farthest away from you and bend it at a right angle.
- Gently pull on the bent knee towards you and carefully roll them onto their side.
- Tilt their head back and lift their chin to open their airway. Ensure nothing is blocking the air passage.
- Stay with them until they fully recover.
If you know they have a hypo and have a glucagon injection or nasal spray with them, administer it promptly (17, 26). However, don’t give them food or drink, as they could choke, including high-sugar preparations to be applied inside their cheek (38).
Can type 2 diabetes make you dizzy?
Yes, too high or low blood sugar—the key characteristic of type 2 diabetes—can cause dizziness. People with type 2 diabetes may also experience vertigo, low blood pressure, and dehydration, all known culprits for that disorienting feeling. Some diabetic medications like insulin may worsen the problem (3, 28, 52).
Can prediabetes cause dizziness?
Prediabetes means you are resistant to insulin, and your blood glucose levels are higher than normal (yet not high enough to be diabetes). The tricky part is you won’t see any noticeable symptoms. This can only be detected by blood sugar testing (34).
However, dizziness, the common symptom of diabetes, maybe a signal that your prediabetes has progressed to type 2 diabetes.
Why do I feel weird after eating sugar?
What’s making you feel this way can be different for everyone. One possibility is when your blood sugar rises quickly and drops rapidly a few hours later (4, 22). This “sugar crash” can bring shakiness, sweating, fatigue, and mood swings (53).
Is dizziness a sign of diabetes? If you urinate often and feel thirsty, it might signal diabetes (21). Yet some may have allergies or sensitivities to ingredients commonly hiding in sugary treats.
What gets rid of dizziness fast?
To alleviate dizziness, find a cozy spot to chill out, sitting or lying down. It helps prevent spills and injury. Next, take deep breaths to calm your body. Drink some water or tea with honey, Ginkgo biloba, cinnamon, and ginger for an extra boost.
It’s crucial to remember that these are just quick fixes, not medical advice.
How do I bring down high blood sugar quickly?
If you have high blood sugar (hyperglycemia), address it swiftly to prevent complications. However, rapidly reducing your blood sugar levels can be dangerous.
To bring down your blood sugar naturally, drinking water to flush excess sugar via urine (20). Gentle and regular exercise can also help your body use glucose more effectively (4). However, avoid intense workouts if your blood sugar is soaring sky-high. They might send it even higher (38).
Summary
Can diabetes cause dizziness? Diabetes and dizziness may go hand in hand due to high/low blood sugar, pressure, and dehydration. Also, check your medications, as many can be the culprits.
Figuring out what’s behind the dizziness is crucial, especially for those managing diabetes, as it could be an early sign of a serious issue.
How to stop dizziness from high blood sugar? You need to keep up with regular checkups and change your lifestyle. Don’t forget some handy home remedies like honey, Ginkgo biloba, ginger, cinnamon, and the Epley maneuver technique.
If you have diabetes and often have dizziness, talk to your doctor. Ignoring these episodes can lead to serious complications.
















Comments
0